Pelvic Exam | Vibepedia
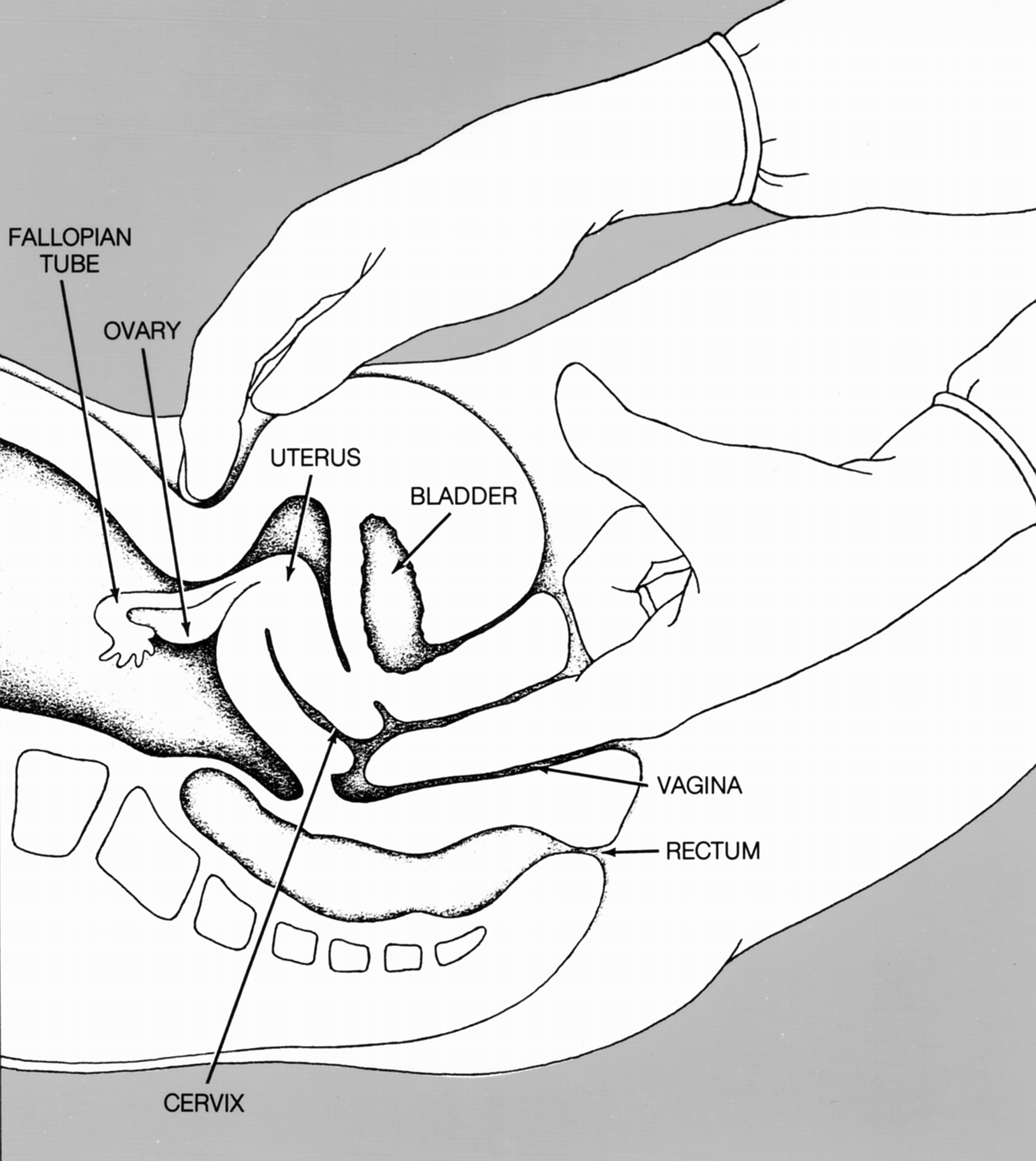
The pelvic exam is a fundamental diagnostic procedure in gynecology, involving the external and internal examination of female pelvic organs. It's crucial for…
Contents
Overview
The origins of the pelvic exam are deeply intertwined with the development of gynecology as a medical specialty, particularly in the late 19th and early 20th centuries. Early gynecological practices, often performed by male physicians, laid the groundwork for the systematic examination of female reproductive organs. J. Marion Sims' methods were notoriously experimental and ethically questionable, involving enslaved women. The widespread adoption of the speculum allowed for direct visualization of the cervix, transforming diagnostic capabilities. The Pap smear further cemented the pelvic exam's role in preventative care, shifting its focus from purely diagnostic to screening. The procedure, however, remained largely standardized without significant input from patients for decades, contributing to its often uncomfortable reputation.
⚙️ How It Works
The standard pelvic exam involves three primary components, typically performed sequentially. First, the external exam assesses the vulva, perineum, and anus for any abnormalities like lesions, swelling, or discharge. Second, the bimanual exam involves the clinician inserting one or two gloved, lubricated fingers into the vagina while the other hand presses gently on the lower abdomen. This allows for palpation of the uterus, ovaries, and fallopian tubes, assessing their size, shape, position, and tenderness. Finally, a speculum, a duck-billed instrument, is inserted into the vagina to gently separate the walls, allowing visualization of the cervix. During this phase, a cytobrush or spatula may be used to collect cervical cells for a Pap test or other tests for STIs.
📊 Key Facts & Numbers
Globally, an estimated 70-80% of women aged 18-65 undergo a pelvic exam annually, though this rate can vary significantly by region and healthcare access. The Pap test, a common component, screens for HPV and precancerous cervical changes; in the US, the recommended screening interval for women aged 21-65 is every three years with cytology alone, or every five years with co-testing for HPV. The global market for gynecological diagnostic devices, including speculums and cytology brushes, was valued at approximately $2.5 billion in 2023 and is projected to grow. Studies indicate that up to 40% of women report experiencing some level of discomfort or pain during a pelvic exam, with higher rates among those with a history of sexual trauma or PID.
👥 Key People & Organizations
Key figures in the history of the pelvic exam include J. Marion Sims, whose controversial early work on vaginal fistulas paved the way for internal examinations, and George Papanicolaou, inventor of the Pap test. Organizations like the American College of Obstetricians and Gynecologists (ACOG) and the Royal College of Obstetricians and Gynecologists (RCOG) establish clinical guidelines and best practices for performing pelvic exams. The Planned Parenthood federation plays a significant role in providing accessible gynecological care, including pelvic exams, to millions worldwide. More recently, patient advocacy groups like It's On Us have pushed for greater patient autonomy and trauma-informed care within medical settings, influencing how exams are conducted.
🌍 Cultural Impact & Influence
The pelvic exam has become a cultural touchstone, often depicted in media as a rite of passage into womanhood or a source of significant anxiety. Its intimate nature has made it a subject of discussion in feminist discourse, exploring issues of bodily autonomy, medical power dynamics, and patient consent. The procedure's association with sexual health and reproductive rights has also placed it at the center of broader social and political debates. For many, the exam represents a necessary but often dreaded encounter with the healthcare system, shaping perceptions of medical authority and personal vulnerability. The cultural perception is further complicated by its necessity for routine health maintenance versus its potential for discomfort or trauma.
⚡ Current State & Latest Developments
Current developments in pelvic exam practices focus on enhancing patient comfort and improving diagnostic accuracy. Innovations include the development of self-sampling kits for HPV testing, which can reduce the need for in-clinic speculum exams for certain screenings. Research is also exploring the use of AI in analyzing cervical cell samples to improve detection rates for precancerous lesions. Furthermore, there's a growing emphasis on trauma-informed care protocols, encouraging clinicians to explain each step, obtain explicit consent, and offer options like having a chaperone present. The telemedicine revolution is also beginning to influence gynecological care, though direct physical examination remains critical for many diagnoses.
🤔 Controversies & Debates
Significant controversies surround the pelvic exam, primarily concerning its routine necessity and the potential for patient distress. Critics argue that the exam is overused, particularly in asymptomatic individuals, and that the benefits of routine screening for certain conditions, like ovarian cancer, have not been definitively proven to outweigh the risks and discomfort. The issue of unnecessary pelvic exams has been a subject of debate among medical professionals and patient advocates. Additionally, the historical context of the exam, particularly its origins in practices that lacked adequate consent, continues to fuel discussions about patient rights and the power dynamics inherent in the clinician-patient relationship. The potential for exams to re-traumatize survivors of sexual assault is another critical point of contention.
🔮 Future Outlook & Predictions
The future of the pelvic exam is likely to involve a greater integration of technology and a more patient-centered approach. We may see a continued shift towards at-home testing for certain screenings, reducing the frequency of in-person speculum exams. The development of VR or augmented reality tools could potentially aid in clinician training and patient education, demystifying the procedure. Furthermore, ongoing research into non-invasive diagnostic methods for gynecological conditions could eventually supplement or even replace certain aspects of the traditional exam. The emphasis will undoubtedly remain on shared decision-making, ensuring patients are fully informed and comfortable with the care they receive, potentially leading to more personalized and less anxiety-provoking examinations.
💡 Practical Applications
The primary application of the pelvic exam is in routine gynecological care, serving as a vital tool for screening and diagnosis. It is essential for detecting cervical cancer via the Pap test, screening for STIs through swabs and cultures, and diagnosing conditions such as endometriosis, uterine fibroids, ovarian cysts, and PID. The exam is also critical in cases of sexual assault for forensic evidence collection and medical assessment. Furthermore, it plays a role in prenatal care to assess pelvic structure and in managing conditions like infertility or urinary incontinence.
Key Facts
- Category
- science
- Type
- topic